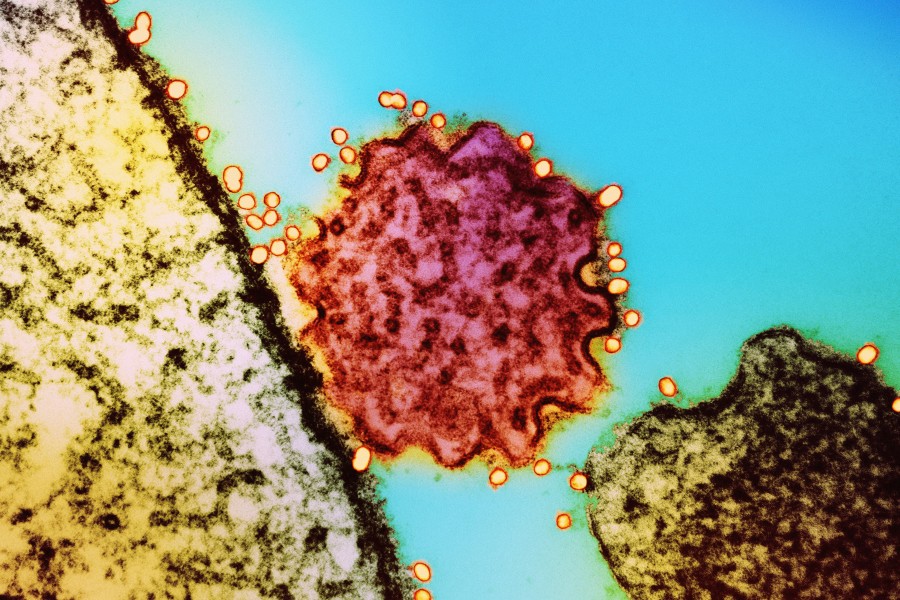
Nipah Virus
Nipah is a bat virus that causes occasional zoonotic outbreaks, most of which are associated with the seasonal consumption of foodstuffs contaminated with bat urine. The case fatality rate is high, but the virus does not transmit effectively person to person.
Nipah is a location-specific hazard for regions where contact with bat-contaminated environments might occur, and so production risk is limited to filming in specific geographic areas.
There is no credible risk to productions filming in the UK, Europe, North America, or in urban studio environments.
Where Nipah Is Relevant
Risk is confined to rural parts of South and Southeast Asia, particularly Bangladesh, Kerala, West Bengal and – historically – parts of Malaysia. There was a recent small cluster in West Bengal associated with health care workers.
Risk increases only where filming involves:
- Areas with large fruit bat populations
- Outdoor rural locations
- Agricultural settings
- Traditional food collection practices (e.g. date palm sap)
This is another example where increased human encroachment into bat habitats due to deforestation, agricultural expansion and settlement brings people, livestock, and virus reservoirs into closer contact, increasing the likelihood of these rare spillover events.
How Transmission Occurs
Nipah does not spread casually or through the environment at large. Transmission pathways of relevance to productions are:
- Direct contact with infected animals like bats, pigs or horses
- Consuming fruit or fruit products such as raw date palm juice that has been contaminated with infected bat saliva or urine. In some outbreaks, domestic animals – most notably pigs – have acted as intermediate hosts, transmitting the virus to humans through close contact.
- Nipah virus can spread between people through close physical contact / exposure to respiratory secretions or other bodily fluids of an infected individual, most often within households or healthcare settings. However, the virus does not transmit easily between people.
Nipah is not airborne and does not spread through brief proximity or passing contact.
The current outbreak does not appear larger or more severe than previous Nipah outbreaks. Similar past outbreaks have involved small clusters with limited human-to-human transmission. Risk to productions is low to moderate only for rural location filming in affected regions.
Practical Controls for Productions
Where filming occurs in known Nipah regions, sensible controls are sufficient.
Location Planning – avoid filming under bat roosting trees, night shoots in areas with heavy bat activity and agricultural buildings used by bats.
Food & Drink Safety: do not consume locally collected raw date palm sap; use sealed, commercially bottled drinks. Ensure catering is bat-proofed and covered. Ensure fruit is washed and do not eat it if its skin is broken.
Cast & Crew Briefing: discuss local transmission routes, emphasise hand hygiene, avoid unnecessary contact with wildlife.
Medical Planning: identify local medical facilities in advance and have a clear reporting pathway for febrile or neurological symptoms. No special PPE is required beyond normal hygiene measures.
Productions do not need:
- Respirators or masks specifically for Nipah
- Vaccination (none available)
- Production shutdowns unless advised by local public health authorities
- Enhanced controls outside affected regions
But it’s in the same family as measles…
Yes it is, and measles spreads famously well. But viral transmission isn’t determined by family name. It’s driven by where a virus replicates, how it exits the body, how stable it is in air, and how much virus is shed, and across this family alone there are nearly 100 species with wildly different transmission profiles.
Being in the same family tells us about evolutionary history, not epidemic risk. There is no biological or epidemiological evidence that Nipah could transmit like measles, and decades of outbreak data actively contradict that claim.
Bangladesh and India experience Nipah outbreaks almost every year. Across all of them, we have never seen sustained airborne transmission or exponential community spread. If Nipah had measles-like transmission, repeated outbreaks in densely populated regions would have produced explosive regional – and likely global – spread decades ago. They haven’t.
Measles is an extreme outlier; it’s exceptional, even among respiratory viruses. It has an R₀ of ~12 to 18, remains airborne for hours, has a very low infectious dose and is shed in enormous quantities from the upper respiratory tract. Very few pathogens across any virus family come close to this combination of traits.
Nipah virus behaves very differently. Primary transmission is directly from fruit bats to humans, or via food contaminated by bats. Human-to-human transmission can occur, but it is limited and inefficient, typically requiring close, prolonged contact such as caregiving. It has never shown the characteristics needed for widespread airborne spread.
So, same family, very different biology – and there are key differences that matter much more than the family name:
| Feature | Measles | Nipah |
|---|---|---|
| Primary site of replication | Upper respiratory tract | Often deep tissues |
| Airborne stability | Very high | Low |
| Infectious dose | Extremely low | Higher |
| Asymptomatic spread | Common | Rare |
| Sustained community spread | Yes | No |
Viral transmission is driven by where the virus replicates, how it exits the body, and how stable it is in air – not its family name.
Nipah being in the same family as measles tells us about evolution, not epidemic risk. There is no biological or epidemiological basis for claims Nipah could spread like measles, and decades of outbreak data directly contradict the idea.
Nipah Virus | International Advice
326
Article last updated on Feb 11th, 2026









